Innovations for Integrated Diagnostics Systems (Round 19)
The Opportunity
Diagnostic services are essential to guide patient treatment and care for a variety of health conditions. In the developing world, diagnostic services range from centralized laboratory settings in highly populated regions to remote health outposts that have limited resources Figure 1. A well implemented centralized laboratory has the potential to achieve high throughput testing with multi-purpose platforms, often at low cost. To date, the function of existing laboratory services in the developing world remains poor due to multiple factors including low instrument utilization rates, poor data management, supply chain issues, human resource challenges, low rates of results returned, poor quality systems, poor sample transportation systems and low quality specimens.
The obstacles to making this a reality include but are not limited to the following areas:
Connectivity: one of the key failures of local testing is due to the fact the sample drawing, patient data, test results are either recorded on paper based systems or not recorded at all. As a result, it is difficult to monitor the effectiveness of local testing thus preventing actionable review.
Sample Collection & Specimen Processing: many test results are wrong or inconclusive due to the fact that the specimen was collected in insufficient quantities or was not stabilized for analysis by the intended centralized lab test.
Transportation & Distribution of Samples: transportation of stabilized specimens can extend the reach of many centralized laboratory services. In the current situation, there is an inadequate transport network to move samples between the clinic where care is taking place and the centralized lab.
Simplified/Streamlined Workflow: numerous high performance testing platforms and assays work well in a setting with abundant resources and highly trained personnel. When these same platforms are used in a resource limited setting, their performance suffers.
The Challenge
Our challenge is to make technological and process improvements in all the areas mentioned above, while at the same time paying attention to balance the cost trade-offs.
- Optimize transportation networks, and leverage distribution capabilities from other local services to improve sample transport logistics, timelines, and cost.
- Adapt selective centralized laboratory instrument platforms and assays that improve ease of use or robustness in developing world settings.
- Seek novel ways to implement interconnected laboratory networks that will efficiently track patients, specimens and data to and from various types of settings, ensuring quality diagnostic services are provided and can inform treatment and care decisions.
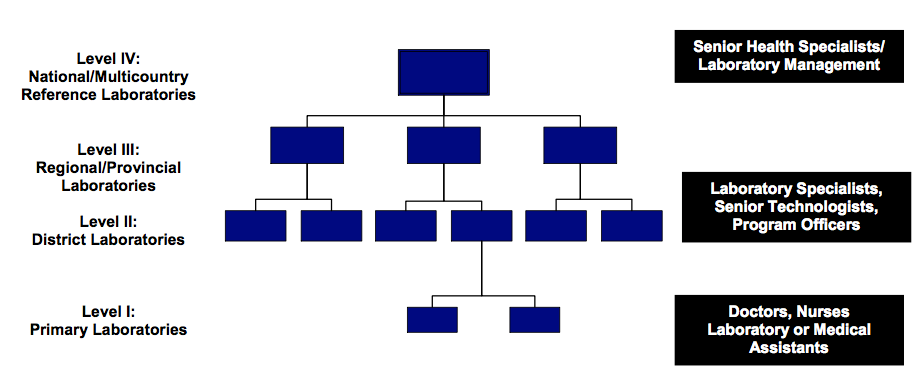
Figure 1. The Tiered, Integrated Laboratory Network;
Because financing for healthcare in the developing world is limited, for any new technology to scale, it must demonstrate cost savings and increased efficiency to the system overall. To balance the cost trade-offs and efficiently manage services, interconnected and coordinated systems from specimen collection, local testing, sample transportation, centralized testing and return of results must be in place.
What we are looking for:
Technical innovations that have a measurable improvement in an integrated laboratory network, starting from sample collection, transportation, laboratory testing (local or centralized) to return of the results. Innovations should have the potential to improve turn-around time (from specimen collection to return of result), laboratory instrument capacity utilization rate, percentage of quality results generated, percentage of quality results returned or cost per quality result returned. Early stage feasibility studies are encouraged.
Options to be considered include:
- Improved reagents for centralized lab tests enabling greater robustness to developing world conditions, improving percentage of quality results generated.
- Improved usability of existing laboratory processes, such as an integrated sample processing device, improving the laboratory instrument capacity utilization.
- Technology that can stabilize specimens during collection and transportation, improving the quality of the results generated.
- Technology that can improve ease of specimen collection such as simpler blood or plasma collection systems, improving quality of results generated.
- Novel methods of improving the transportation network such as digital trackers or apps that improve sample transportation, reducing turn-around times.
- Patient-managed data systems, with secure and easily accessible information that patients can contribute to themselves, enabling better access and result return.
- Methods to identify patients who may not have a unique identification number, consistent demographic information or visit multiple clinic sites, ensuring high percentage of results returned.
To be considered for funding, proposals must clearly describe how the proposed innovation would work within and improve existing laboratory networks. Estimates of current wastage that could be improved, a description of how the technology could improve a component of the entire system, a description of how the improvement could eventually be demonstrated, will be required for a proposal to be reviewed.
We will not consider funding for:
- Any technology that is currently used in the developing world setting for improvement of diagnostic services
- Point of care diagnostics instruments
- New diagnostic laboratory instrumentation
- Implementation or scaling of existing solutions
- Innovations that cannot demonstrate impact on efficiency